PCR Release Testing for Mycoplasmas Gaining Ground versus Conventional Methods
Biomanufacturing contamination is a very real concern for biopharmaceutical companies. Manufacturing shut downs due to contamination can result in regulatory fines, drug shortages, and medication rationing. In addition, lost revenue and lost market share can leave companies vulnerable and at risk of serious loss of stock value. While any contamination can be extremely challenging and costly, mycoplasma contamination is particularly difficult.
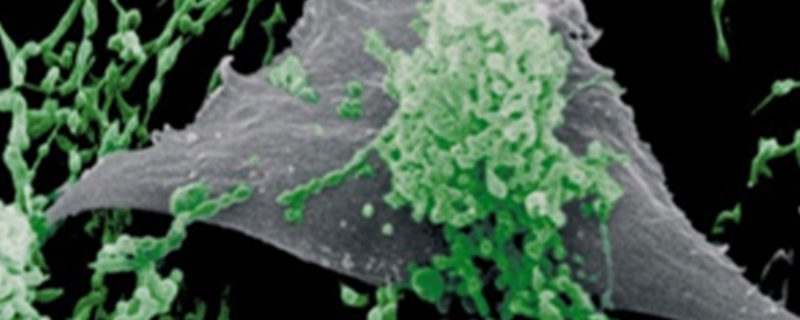
Mycoplasma Photo: © R. Rosengarten, Mycosafe, courtesy of Roche
Why is Mycoplasma such a challenge?
Pervasive
Mycoplasma contamination is a pervasive threat. According to the publication” The scope of mycoplasma contamination within the biopharmaceutical industry, “contamination rates in established cell cultures have been reported between 15 and 35% with considerably higher occurrence cited in certain selected populations.” Its pervasiveness could be due to several different reasons, but one is certainly due to the fact that mycoplasmas can have a broad range of hosts – including humans, animals, insects and plants. Common sources of contamination consist of cell culture raw materials including media, sera, and supplements, particularly if these are sterilized using filtering because mycoplasmas are too small to be caught by most standard filters. In addition, mycoplasmas can be brought in through new cell banks, which makes pre-screening a must. Even lab personnel can be carriers of mycoplasmas and can inadvertently contaminate a culture.
Antibiotic Resistance
Mycoplasmas are small bacteria that lack cell walls. This lack of a cell wall makes them resistant to many common antibiotics that target the cell wall as the mechanism of action.
Difficult to Detect
The small size of mycoplasmas makes them difficult to detect and they are not detectable by light microscopy. Mycoplasmas tend to thrive in cell culture environments because they find nutrients in host cells and can grow to high concentrations without causing any obvious problems in the culture. Eventually, of course, if left unchecked they can destroy an entire cell line.
Release Testing Requirements
Biopharmaceuticals must be completely free of mycoplasmas and regulatory authorities require release testing as part of the manufacturing process. Traditional methods for mycoplasma testing as described in the USP (U.S. Pharmacopeial Convention) and EP (European Pharmacopoeia) involve a combination of cell culture in the form of agar culture and broth culture and indicator cell testing. Current limit of detection accepted by regulatory bodies is 10 CFU/ml or less for all mycoplasma strains tested.
These testing methods, while well defined and widely accepted, are difficult to administer because they require highly trained personnel to administer and can require up to 28 days for results. As a result, there is a strong desire to find the most effective system for detection. In response, PCR testing for mycoplasma has been developed. However, this method must be able to prove sensitivity comparable to the traditional methods outlined by the USP and EP and accepted by the regulatory authorities.
PCR Solution
PCR mycoplasma tests are not a new idea, the first kit design was developed in the early 2000’s, but testing has been refined, improved and now put through the rigors of use in a pharmaceutical approved by a regulatory body. Use of PCR mycoplasma detection kits falls under the E.P. 2.6.7 Guidelines for NAT Detection of Mycoplasmas. It is important to note that regulatory authorities do not approve the commercial kits and it falls to the sponsor company to prove equivalence with traditional methods as part of the complete control strategy.
PCR mycoplasma detection is gaining in popularity and is now accepted in the EU, Japan and many other countries. The FDA has also approved biopharmaceuticals using PCR mycoplasma testing instead of traditional testing methods as part of the overall control strategy.
Roche recently hosted an interesting webinar on the evolution of their MycoTOOL kit – “Achieving FDA Acceptance and Releasing Your BioProduct with MycoTOOL PCR Mycoplasma Detection Kit.”. It was of particular interest because of the ability to follow this test through the pharmaceutical approval process as part of the overall control strategy. Roche is uniquely positioned to be able to provide both the perspective of developing the PCR test and also of implementing their MycoTOOL on the Pharma side of Roche as part of their control strategy for one of their pharmaceuticals. The result was a candid discussion of the issues raised by regulatory bodies and how they addressed each issue. Roche described the scientific rationale and experiments conducted to demonstrate comparability to traditional methods and ultimately acceptance for use of MycoTOOL in the release of their pharma product.
Roche reported the following 5 most critical questions asked of Roche Pharma by the regulatory authorities.
- Question: Is the sample’s homogeneity ensured? Is 1 ml representative?
Response: Roche was able to demonstrate that a small sample volume like 1 ml is representative. - Question: Does freezing/thawing influence the viability of mycoplasma stocks?
Response: Roche was able to show that freezing/thawing has no influence on detection limit. - Question: Are conventional cell culture and PCR methods comparable?
Response: Roche through extensive testing demonstrated that the MycoTOOL test using PCR is fully comparable to classical methodology. - Question: Can MycoTOOL detect species beyond the tested ones?
Response: Extensive primer alignment data proved all relevant species detectable. - Question: How is the GC/CFU ratio tested?
Response: Most mollicute reference stocks have a GC/CFU ration of <100.
The speaker then walked through how each of these questions was addressed with the regulatory authorities. Thus paving the way for future use of this method for release testing.
Summary
There are several commercially available PCR based mycoplasma detection kits available for purchase. For anyone interested in learning more about the use of PCR based mycoplasma release testing in their manufacturing, I would recommend the Roche webinar. The webinar provides a good overview of the use of PCR in testing for mycoplasma, advantages over traditional methods, and also what to expect in terms of demonstrating comparability for regulatory authorities.
